Case Reports – Documented Success Stories!
Case Report 1: Toe ulcer after failed bypass
“Treatment of non-reconstructable PVD with the Arterial Assist Device”
Paul S. van Bemmelen, MD, Stony Brook, NY and Valerie A. Brunetti, DPM, Northport, NY
Patient
- 68 y.o. male with diabetes
- 4-month history of rest pain and progressive necrosis
- PVR’s were diminished, flat wave form at toe level
- No run-off towards the toe
ArtAssist® Device
- Applied intermittent compression to foot, ankle and calf at 120mmHg
- Home use 1 hour, q.i.d.
- Metatarsal PVR-amplitude increased
- The lesions are almost healed (second toe completely healed)
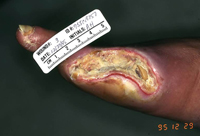
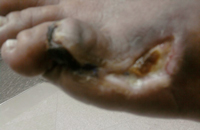
Patient is a 68-year-old man with diabetes; status post Coronary Artery Bypass Graft (CABG), Cartoid Endarterectomy (CEA) and bilateral femoro-popliteal bypass and bilateral profundaplasty. Patient presented with a 4-month history of rest-pain and progressive necrosis of the right hallux (figure 1).
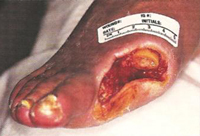
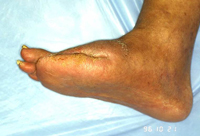
A small lesion was developing on the tip of the second toe. Non-invasive pulse-volume recording (PVR) demonstrated a diminished amplitude of 3mm at the metatarsal level, with a flat waveform at the toe level. Arteriography demonstrated patent vessels down to the ankle, but no run-off towards the forefoot (figure 2). Patient used ArtAssist® compression for one hour, q.i.d. Topical treatment consisted of a non-adherent dressing only and minor debridements in the office. After completion of a 3-month compression protocol, the lesions were almost healed (figure 3). Metatarsal PVR-amplitude increased to 9mm. Note the tip of the second toe, which was already healed after one month.
ArtAssist® can increase skin-flow more than 4 times.1,2
References:
- van Bemmelen PS, Weiss-olmanni J, Ricotta JJ: Rapid intermittent compression increases skin circulation in chronically ischemic legs with infra-popliteal obstruction. VASA 2000;29:47-52.
- Eze AR, comerota AJ, et al. Intermittent calf and foot compression increases lower extremity blood flow. Am J Surg. 1996;172:130-135.
Download a pdf of ArtAssist® Case Report 1
Case Report 2: Diabetic with Renal Failure
“Diabetic limb salvage using the Arterial Assist Device… ArtAssist®”
Paul S. van Bemmelen, MD. PhD, Port Jefferson, NY and Gerald J. Furst, DPM, Port Jefferson, NY
Patient
- 66 Year Old Male
- 35 Year Hx of diabetes
- Renal Failure
- Contralateral Tibial Bypass
- Poor Ambulation
- Small Vessel Disease
Past Therapies
- Amputation Great Toe/Metatarsal I
- Platelet Released Growth Factors
- IV and Oral Antibiotics
- Topical Antibiotics
- Surgical Debridements
ArtAssist® Device
- Applies Compression to Foot, Ankle and Calf Up to 100 mmHg
- Home use for 30 min. QID
- Improved Circulation
- Prepared Foot For Revision Surgery
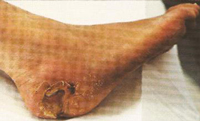
A 66-year-old man with a 35 year history of diabetes (NIDDM) and chronic renal failure (peritoneal dialysis) presented with dry necrosis of his right great toe. He ambulated very little outside of his home and he had previously undergone a tibial bypass of the opposite leg. He was being treated with platelet released growth factors for poor healing of his left distal ankle incision. Ankle blood pressure was not obtainable due to non-compressibility, but waveforms were consistent with disease of the small vessels distal to the knee. The metatarsal pulse volume recording is shown (Fig. 1) and is essentially flat. Toe-pressure was in the ischemic range.
The patient underwent repeated selective digital intra-arterial angiography, which demonstrated patent arteries to the level of the ankle only, without named run-off vessels in the foot. After explaining the poor chances of healing of a toe amputation to the patient, he underwent amputation of the right great toe and metatarsal head. Treatment with the ArtAssist® device was not available at that time. The toe amputation failed and complete dehiscence, with exposed metatarsal bone was apparent in debridements and immediate treatment with growth factors were instituted. Further deterioration occurred slowly. Further revision foot amputation was not considered to be a worthwhile option and below-knee amputation would be the next surgical step.
Intermittent compression with the ArtAssist® device was started two months after the toe amputation for at least 30 minutes, QID. Compression was well tolerated and after one week of home treatment, the patient noticed blood on his dressings. Slowly some granulation tissue appeared and the wound edges bled well with minor debridements. Improvement of the metatarsal pulse volume recording was noted. In view of the exposed metatarsal bone, with retracted skin edges, a further resection of Metatarsal I and the adjacent second toes was performed after two months of compression therapy. Oral antibiotics were given based on culture results. The growth factor treatment was stopped. The resulting wound is now healed by secondary intention (Fig 2). Further improvements occurred of the pulse volume recording at the metatarsal level, to the same amplitude as the bypassed side.
Download a pdf of ArtAssist® Case Report 2
Case Report 3: Heel Necrosis with Renal Failure
“Treatment of Non-Healing Lower Extremity Ulceration With a New Form of Progressive, Rapid, Pneumatic Compression”
Nancy D Shebel, MHA, RN, BSN, CVN, RVT and Duane Amundsen, MD, FACS. General Surgery/Section of Vascular Surgery, Kaiser Permanente Medical Center Panorama City, California
Patient
- 36 y.o. male, 20+ years type I diabetes
- Retinopathy and peripheral neuropathy
- Renal failure, 6 years on hemodialysis
- Left below knee amputation
- Large right heel necrotic ulcer
Past Therapies
- Surgical debridements
- IV, oral and topical antibiotics
- Standard wound care treatment
- No runoff vessels for bypass surgery
ArtAssist® Device
- Applies compression to foot, ankle and calf at 120mmHg
- Home use for 30 min.QID
- Increases blood circulation
- Ulcer size decreased substantially
- Limb was saved
We describe a new technology for treating non-healing arterial ulcers and limb salvage. This device increases blood flow by 2 to 4 times in diabetics and other patients with ischemic limbs that are non-surgical candidates.1 We are reporting on a diabetic patient with a non-healing arterial heel ulcer expected to undergo right below knee amputation, since he was not a bypass candidate. The treatment options were amputation or to attempt ulcer healing with this new technology – the ArtAssist®*. Saving his leg would mean he could be fitted with a left leg prosthesis allowing a more normal lifestyle for a relatively young man. It was also a consideration that if the heel ulcer could be healed and the leg saved, he would be considered a candidate for a kidney transplant. ArtAssist® is a home use device that applies rapid progressive pneumatic compression while the patient is seated comfortably in a chair with the treated limb in a dependent position. ArtAssist® rapidly applies 120mmHg pressure beginning at the foot, continuing to the ankle and then the calf, 3 times a minute. The treatment consisted of 4, half hour sessions daily. This compression regimen simulates the beneficial effects of brisk walking, without pain or tissue trauma. Patient compliance is measured with a hidden internal hour metter accessible only to the nurse.The limb was saved, despite the patient’s poor compliance (only 37 min. daily out of the 120 prescribed). Ulcer size decreased substantially over 8 months and complete healing was imminent. After the 8-month visit our patient did not return for any follow-up visits in our department, despite numerous attempts and phone calls to him. Review of the clinical record after his demise 6 months later revealed that the heel ulcer never healed completely, but did not further deteriorate. The final reading from the internal hour meter indicated that the ArtAssist® had not been used since his last visit. Recent clinical trials have proven the efficacy of ArtAssist® for patients with intermittent claudication.2 Patients showed improvement in ankle brachial indices, and increased walking distances. The authors hypothesize these improvements are due to increased collateral circulation. Our experience at Kaiser Permanente supports these findings in our limb threatened ulcer patients.
Conclusion: Any patient presenting with a non-healing ulcer should be considered a candidate for this new therapy. We feel this is an important adjunct in treating our patients with peripheral arterial disease and we advocate its use in non-surgical patients.
References:
- Eze AR, Comerota AJ, Cisek PL, Holland BS, Robb PK, Veeramasuneni R, Comerota Jr. AJ. Intermittent calf and foot compression increases lower extremity blood flow. Society for Clinical Vascular Surgery, 24th Annual Symposium on Vascular Surgery. March 1996.
- Nicolaides AN, et. al. New Horizons and Techniques in Vascular and Endovascular Surgery. 24th Annual Symposium on Current Critical Problems. November 1997.
*ArtAssist® model AA-1000 (ACI Medical, Inc., San Marcos, CA USA). This paper was supported in part by ACI Medical, Inc., San Marcos, CA.
Download a pdf of ArtAssist® Case Report 3
Case Report 4: Diabetic non-healing ulcer
“Healing the Arterial Foot Ulcer using Arterial Pump Technology”
Darwin Eton, MD. Baptist Cardiac and Vascular Institute, Miami, Department of Surgery, University of Miami School of Medicine
Patient
- 67 years old
- Female
- Ex-smoker
- Critical Limb Ischemia
- Well-controlled Type II DM
- Multiple revascularization attempts
- Non-healing ulcer / gangrene
- Standard wound care
- Inadequate vein for bypass
- Distal disease with small target vessels
- Was offered below knee amputation
ArtAssist® Device
- Prescribed ArtAssist® compression for 3 1/2 months, for 3 to 5 hours per day in hourly treatment sessions.
- Ulcer was completely healed and the device has been discontinued.
Download a pdf of ArtAssist® Case Report 4